
Mar 6, 2026
You finish a verbal handoff and sit down to chart, but a few interruptions later the details you meant to record about that patient start to blur. Instead of capturing the conversation while it is fresh, many clinicians end up reconstructing key points from memory or leaving notes too vague to guide the next provider. Learning how to document patient handoffs faster starts with reducing the gap between the conversation and the chart. Structured frameworks like I-PASS or SBAR, combined with real-time documentation and voice-based tools that convert spoken notes into text inside the systems clinicians already use, make it possible to capture the full handoff while the information is still clear.
TLDR:
Structured handoff programs such as I-PASS have been shown to reduce medical errors by 23% and preventable adverse events by 30% in multicenter hospital studies.
One study found dictated clinical notes averaged about 320 words compared with 181 words for typed notes while taking similar time to complete.
Templates for common scenarios can considerably reduce the time required to document handoffs during high-volume shifts.
Protected 15-minute blocks at shift changes prevent rushed documentation and missed critical details.
Certain solutions learn medical terminology over time at 200ms latency with HIPAA compliance for handoff notes.
Why Patient Handoff Documentation Speed Matters
Patient handoffs happen constantly in healthcare. Teaching hospitals see 4,000 daily handoffs. Each one carries risk.
When documentation lags behind verbal communication, critical details get lost. A delayed allergy notation. An unclear medication change. A missed lab result that needed follow-up. These gaps don't just slow down care; they put patients in danger.
Fast documentation isn't about checking boxes faster. It's about capturing accurate information while it's fresh, before the next emergency pulls your attention away. When handoffs take too long to document, you're either rushing through details or cutting into time you need for actual patient care.
The math is simple: faster documentation means more time with patients and fewer errors from memory lapses. Every minute you save on charting is a minute you get back for the work that actually requires your clinical expertise.
Choose the Right Handoff Framework for Your Setting
Structured handoff frameworks give you a roadmap for what to document and in what order. Medical error rates decreased by 23% and preventable adverse events dropped by 30% after structured handoff programs were implemented. Different frameworks fit different settings.
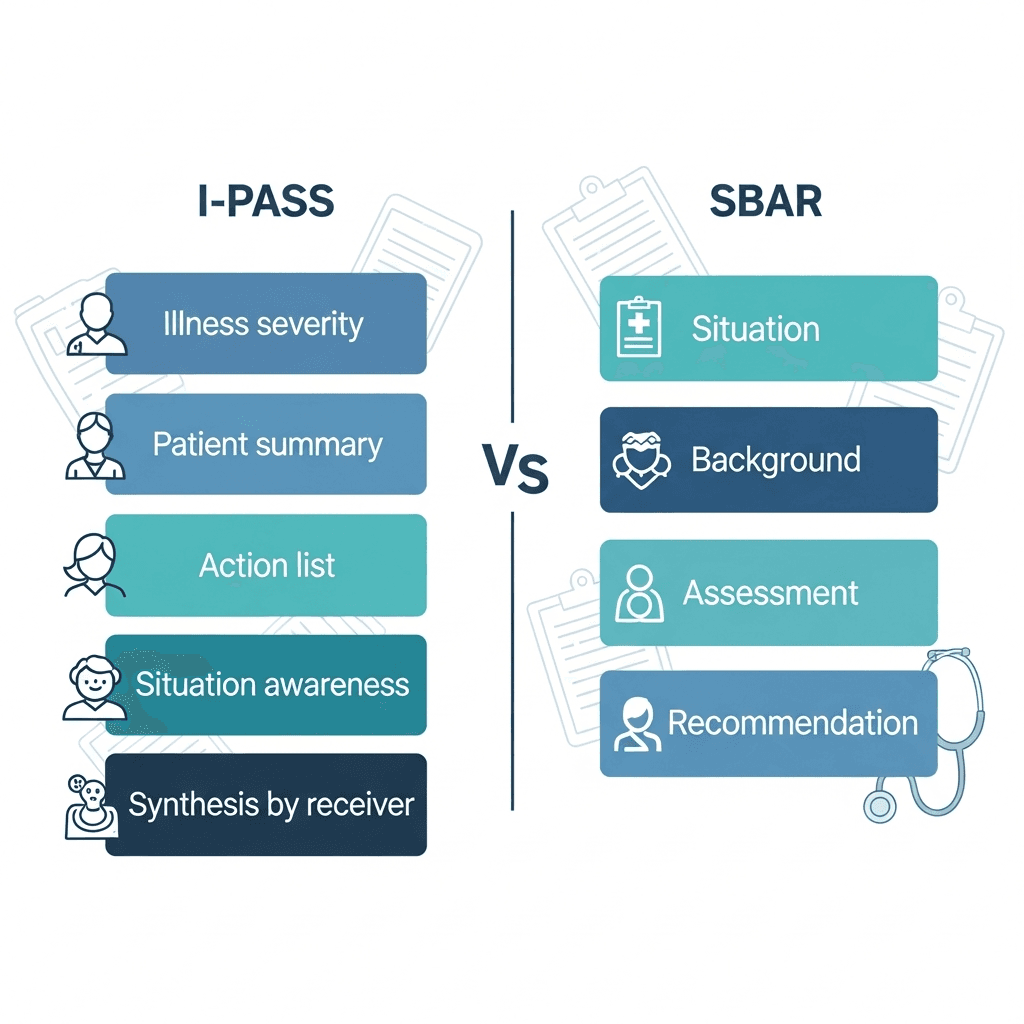
I-PASS works well in teaching hospitals where handoffs involve multiple team members and complex patient histories. It covers Illness severity, Patient summary, Action list, Situation awareness, and Synthesis by receiver. It's thorough but takes more time.
SBAR fits faster-paced environments like emergency departments or outpatient clinics. You document Situation, Background, Assessment, and Recommendation quickly. It's built for speed when you need to hand off information and move immediately to the next patient.
Pick the framework that matches your documentation load and pace.
Feature | I-PASS | SBAR |
|---|---|---|
Components | 5 elements (Illness severity, Patient summary, Action list, Situation awareness, Synthesis) | 4 elements (Situation, Background, Assessment, Recommendation) |
Best For | Teaching hospitals, complex patients, multidisciplinary teams | Emergency departments, outpatient clinics, fast-paced settings |
Documentation Time | Often takes longer due to the structured format | Typically faster due to the concise structure |
Detail Level | Thorough with interactive verification | Concise and action-focused |
Learning Curve | Moderate - requires team training | Minimal - intuitive structure |
Error Reduction | 23% decrease in medical errors, 30% reduction in adverse events | Widely used to standardize clinical communication and improve clarity during handoffs |
Eliminate Distractions during Handoff Communication
Distractions during handoffs create documentation errors. Handoff errors and omissions occurred in 13.1% and 45.1% of cases, respectively, often due to interruptions and noise.
Set up a dedicated handoff zone away from high-traffic areas. A quiet corner works if your team consistently respects it. Post a "Handoff in Progress" sign to prevent non-emergency interruptions.
Silence your phone. Close extra browser tabs. Ask colleagues to hold non-urgent questions for two minutes. These simple steps protect what gets documented accurately versus what gets missed when someone interrupts mid-handoff.
Combine Verbal and Written Documentation Methods
Verbal handoffs alone miss details. Written handoffs alone miss context. You need both working together.

Start with face-to-face communication where you speak through the critical points: active issues, pending tasks, what to watch for overnight. Your colleague asks questions in real time, catches confusing details, and clarifies orders that don't make sense. That verbal exchange catches errors before they happen.
Document those same points in writing while you're still in the handoff conversation or immediately after. Capture the specifics: exact medication doses, timing of the next assessment, which lab results you're waiting for. Written records give the next shift something to reference at 2 AM when memory gets fuzzy.
The combination saves time later. When everything important is both discussed and documented, your colleague doesn't need to call you an hour into their shift asking what you meant.
Build Interactive Verification Into Every Handoff
Interactive verification catches errors before they become problems. When the receiving clinician repeats back what they heard, you both confirm accuracy and identify what needs clarification.
Ask your colleague to summarize after you finish the handoff: "So I'm watching for sepsis signs, rechecking labs at 6 AM, and calling you if her pressure drops below 90 systolic." If they misunderstood, you correct it immediately instead of finding out about the mistake hours later through an incident report.
This adds 30 seconds to your handoff but saves 30 minutes of chart corrections and follow-up calls when information gets missed. The receiver documents accurately the first time because they confirmed understanding while you were still available to clarify.
Use Voice Dictation to Accelerate Documentation
Voice dictation lets you document four times faster than typing. You speak at 150 words per minute. You type at 40. The math makes handoff documentation instantly faster.
Spoken notes captured more detail than typed notes (320.6 words versus 180.8 words) while taking the same time or less to complete. More information in less time means better handoffs without eating into your shift.
During high-volume handoff periods, voice dictation keeps documentation from becoming a bottleneck. You finish charting one patient and move to the next without your hands limiting how fast you can record what matters. Speak the details while they're fresh instead of typing them from memory later when the next three patients need your attention.
Create Standardized Templates for Common Scenarios
Templates for repeat scenarios can considerably reduce documentation time. Instead of writing a post-op handoff from scratch every time, fill in a pre-structured note that already includes the key elements your team needs.
Build templates around your most common handoff types. Post-operative patients need key sign trends, pain management, drain output, and diet advancement. New admissions need chief complaint, relevant history, active problems, and overnight plan. Transfers between units need current status, why they're moving, and what the receiving team should monitor.
Templates work as cognitive shortcuts during busy periods. When you're handing off six patients before leaving, you don't want to remember every documentation element each time. The template reminds you what matters while you focus on the patient-specific details that actually change between cases.
Schedule Protected Time for Shift Changes
Block off 15 minutes at shift change where handoffs take priority over everything except emergencies. When your team knows handoff happens from 7:00 to 7:15, they stop scheduling non-urgent tasks during that window.
Protected handoff time prevents the rushed documentation that happens when you're trying to chart between admissions, phone calls, and medication passes. You sit down, focus on transferring care, and document thoroughly instead of scribbling incomplete notes between interruptions.
Uninterrupted handoffs get finished faster because you're not restarting your thought process every time someone asks an unrelated question. You complete documentation in one focused session instead of three fragmented attempts that each take longer and miss more details.
Train Your Team on Documentation Speed
Training improves handoff documentation speed across your team. When everyone knows the framework elements cold, they stop wasting time figuring out what to document next.
Run monthly sessions on common documentation errors. Show real examples of missed allergy notations, unclear medication instructions, or incomplete pending tasks. Your team learns what mistakes look like before they make them during actual handoffs.
Teach specific time-saving techniques: approved abbreviations, template shortcuts, voice commands for formatting. Skills compound over time. A clinician who learns to document 20% faster this month saves hours across their career while producing higher-quality handoff notes that keep patients safer.
Use AI-Powered Voice Documentation for Healthcare Teams
Willow takes voice documentation further for healthcare teams managing patient handoffs. The personalization learns your medical terminology and writing style over time, so handoff notes require fewer edits during time-sensitive shift changes. At 200ms latency, you document at the speed of thought without waiting for text to catch up during rapid transitions.
For clinics handling patient communication and charting notes, Willow meets SOC 2 and HIPAA requirements while shared shortcuts and custom dictionaries keep terminology consistent across your team. You speak naturally and complete handoff documentation in a fraction of the typing time.
Standard dictation tools like Wispr Flow and Apple's built-in voice dictation lack the medical-specific personalization and team collaboration features that accurate handoff documentation needs.
FAQs
How long does it take to document a patient handoff using voice dictation?
Voice dictation lets you document at 150 words per minute compared to 40 words per minute with typing, cutting handoff documentation time by roughly two-thirds. Most clinicians complete a standard handoff note in under two minutes when speaking instead of the typical five to seven minutes required for typing.
When should I implement interactive verification during handoffs?
Add interactive verification to every single handoff by having the receiving clinician repeat back critical details like medication changes, pending labs, and monitoring parameters. This 30-second step prevents hours of chart corrections and dangerous miscommunications later.
Why do I need both verbal and written handoff documentation?
Verbal communication lets your colleague ask real-time questions and catch confusing details before errors happen, while written records provide a reference at 2 AM when memory gets fuzzy. The combination prevents follow-up calls and keeps critical details from getting missed hours into the next shift.
Final Thoughts on Improving Patient Handoff Documentation Speed
Improving handoff documentation speed comes down to capturing information while the conversation is still clear and removing the friction that slows charting after shift changes. Structured frameworks like I-PASS or SBAR give teams a consistent format, while templates, protected handoff time, and interactive verification keep documentation accurate without extending the process. The final step in how to document patient handoffs faster is closing the gap between what clinicians say and what appears in the chart. Tools like Willow support this workflow by converting spoken handoff details into structured notes inside the systems clinicians already use, helping teams document transitions quickly while maintaining clear records for the next provider in the care chain.









